What is a colorectal cancer prognosis?
The prognosis for colorectal cancer refers to the likely course and outcome of the disease. It typically involves predicting the chances of survival and the likelihood of the cancer returning after treatment. A prognosis is often assessed based on factors such as the stage of cancer at diagnosis, the tumour’s size and location, whether it has spread to nearby lymph nodes or distant organs, the tumour’s genetic characteristics, and the patient’s overall health and response to treatment.
The prognosis for colorectal cancer can vary widely depending on these factors. For localised cancers (those confined to the colon or rectum), the prognosis tends to be more favourable, with higher survival rates. However, if the cancer has spread regionally or distantly, the prognosis becomes more guarded, with lower survival rates.
Medical professionals may use various tools and systems to predict prognosis, including cancer staging systems like the TNM staging system and prognostic scoring systems that incorporate multiple factors to estimate outcomes. It’s essential to consult healthcare providers for an accurate assessment of an individual’s prognosis for colorectal cancer, as it can vary significantly from person to person. Early detection through bowel cancer screening and prompt treatment can positively impact the prognosis and overall outcomes.
What is colorectal cancer and what is the importance of understanding a prognosis?
Colorectal cancer is a significant health concern worldwide, characterised by the abnormal growth of cells in the colon or rectum. It ranks among the most common cancers globally, with a substantial impact on morbidity and mortality. Understanding the prognosis of colorectal cancer is paramount for patients, caregivers, and healthcare providers alike.
Colorectal cancer, often referred to as bowel cancer, is a type of cancer that starts in the colon or rectum, which are parts of the digestive system. It typically develops from abnormal growths of tissue known as polyps, which can become cancerous over time. Colorectal cancer can affect both men and women and is more common in older adults.
Prognosis refers to the likely course and outcome of the disease, including survival rates and the potential for recurrence. It’s crucial to recognise that prognosis can vary greatly among individuals diagnosed with colorectal cancer, influenced by factors such as cancer stage, tumour characteristics, and overall health status.
Early detection and prompt treatment are key factors in improving colorectal cancer outcomes. Screening tests like colonoscopies can detect precancerous growths or early-stage cancers when treatment is most effective. Moreover, advancements in treatment modalities, including surgery, chemotherapy, and targeted therapies, have significantly improved survival rates and quality of life for many colorectal cancer patients.

What are the types of colorectal cancer?
Adenocarcinoma
This is the most common type, accounting for approximately 95% of colorectal cancer cases. It originates in the glandular cells lining the colon or the rectum.
Carcinoid tumours
These are rare tumours that develop from hormone-producing cells in the digestive tract; they are slow-growing and asymptomatic and require testing.
Gastrointestinal stromal tumours (GISTs)
These can occur anywhere and begin in the GI tract, the colon, and the rectum and tend to form in the stomach and small intestine.
Lymphomas
Cancers of the lymphatic system can affect the colon or rectum. The cure rate is higher, approaching 90%, in younger patients and with early-stage detection.
What are the risks of colorectal cancer?
Family history
Individuals with a family history of colorectal cancer or certain genetic syndromes are at higher risk.
Dietary factors
Obesity, a diet high in red and processed meats, and a low fibre intake can increase the risk of cancer.
Lifestyle factors
Chain smoking, heavy alcohol consumption, and a lack of physical activity can increase the risk of cancer.
Some medical conditions
Diabetes, radiation therapy for prior cancers, and some inherited gene mutations can elevate the risk.
What is the importance of early awareness and diagnosis?
Colorectal cancer is one of the most common cancers worldwide, with approximately 1.9 million new cases diagnosed annually. It ranks as the third most commonly diagnosed cancer in men and the second in women. In 2020 alone, there were over 1.9 million new cases and nearly 935,000 deaths attributed to colorectal cancer globally.
Early detection of colorectal cancer is crucial for improving outcomes and reducing mortality rates. Screening tests, such as colonoscopies, faecal occult blood tests (FOBTs), and stool DNA tests, can detect precancerous polyps or early-stage cancers when treatment is most effective. Despite the availability of screening methods, many cases of colorectal cancer are diagnosed at later stages, emphasising the importance of raising awareness about the disease and encouraging individuals to undergo regular screening as recommended by healthcare guidelines.
By increasing awareness of colorectal cancer risk factors, symptoms, and screening options, individuals will be empowered to take proactive steps towards early detection, leading to better treatment outcomes and ultimately saving lives.
What are the factors influencing cancer prognosis?
The prognosis for colorectal cancer is influenced by various factors, each playing a critical role in determining the outlook for individuals diagnosed with the disease. Understanding these factors can help patients and healthcare providers make informed decisions regarding treatment and care.
Cancer stage
The cancer stage refers to the extent and spread of the disease, including the size of the tumour and whether it has spread to nearby lymph nodes or distant organs. Generally, earlier-stage colorectal cancers have a more favourable prognosis compared to later-stage cancers. Staging helps predict the likelihood of cancer recurrence and guides treatment decisions.
Tumour size and location
The size and location of the tumour within the colon or rectum can impact the cancer prognosis. Larger tumours may indicate a more advanced disease stage and a higher risk of metastasis. Tumours located in certain areas of the colon or rectum may be more challenging to tackle and treat through surgical intervention or may have a higher likelihood of recurrence.
Lymph node involvement
The presence of cancer cells in nearby lymph nodes indicates regional spread and can worsen the prognosis. Lymph node involvement is an essential factor in cancer staging and treatment planning and can guide decisions regarding the need for adjuvant therapies such as chemotherapy or radiation to target any remaining cancer cells and reduce the risk of disease progression.
Metastasis
Metastasis is when cancer cells spread from the colon or rectum to distant organs such as the liver, lungs, or bones. The presence of metastatic disease significantly worsens prognosis and reduces survival rates. Metastatic colorectal cancer often requires more aggressive treatment approaches, such as chemotherapy, targeted therapy, or surgery to remove metastases.

Tumour biology and genetic factors
Certain molecular characteristics of colorectal tumours, such as microsatellite instability (MSI) status and mutations in genes like KRAS and BRAF, can influence cancer prognosis and treatment response rates. Understanding the tumour’s biological features through genetic testing can help tailor treatment strategies and predict outcomes more accurately and efficiently.

Patient-related factors
Patient-related factors, including age, overall health status, comorbidities, and response to treatment, can impact prognosis. Younger patients and those in good overall health tend to have better outcomes. Adherence to treatment plans, lifestyle factors (such as smoking cessation and a healthy diet), and access to supportive care services also influence prognosis.
By considering these factors in conjunction with each patient’s unique circumstances, healthcare providers can develop personalised treatment plans aimed at maximising outcomes and improving the quality of life for individuals diagnosed with colorectal cancer. Early detection through screening and prompt intervention remain crucial in achieving the best possible prognosis for colorectal cancer patients.
What is TNM staging?
The TNM staging system is a crucial tool used to stage colorectal cancer, providing valuable information about the extent of the disease and guiding treatment decisions.
Tumour (T)
This indicates the size and extent of the primary tumour. Tumour staging ranges from T0 (no evidence of tumour) to T4 (tumour has invaded nearby organs or structures).
Node (N)
The involvement of nearby lymph nodes by cancer cells. Lymph node staging ranges from N0 (no lymph node involvement) to N2 (cancer cells present in multiple nearby lymph nodes).
Metastasis (M)
Indicates whether the cancer has spread to distant organs or tissues beyond the colon or rectum. Staging ranges from M0 (no distant metastasis) to M1 (distant metastasis present).
The combination of these factors determines the overall stage of colorectal cancer, which ranges from stage 0 (early, localised cancer) to stage IV (advanced cancer that has spread to distant organs).
What do the cancer stages mean?
Stage 0
Cancer cells are confined to the inner lining of the colon or rectum, with no invasion into deeper layers.
Stage I
Cancer cells have grown and formed through the inner lining but have not spread beyond the colon or rectum.
Stage II
Cancer has invaded through the wall of the colon or rectum but has not spread to lymph nodes or other organs.
Stage III
Cancer cells have spread to nearby lymph nodes but have not spread to distant organs within the body.
Stage IV
The final stage where cancer cells have spread to distant organs or tissues, such as the liver, lungs, or bones.
Accurate staging helps healthcare providers tailor treatment plans to individual patients, providing the best chance for optimal outcomes.
What are some survival rate statistics?
Survival rate statistics for colorectal cancer vary based on the stage at diagnosis.
Localised (stage I)
Approximately 90% of patients survive five years or more after diagnosis when the cancer is confined to the colon or rectum and has not spread to nearby lymph nodes or other organs.
Regional (stage II and III)
Survival rates for regional cancer, where the cancer has spread to nearby lymph nodes but not to distant organs, range from around 70% for stage II to 60% for stage III over five years.
Distant metastasis (stage IV)
For colorectal cancer that has spread to distant organs or tissues, the five-year survival rate drops significantly to approximately 15% or less, reflecting the advanced stage of the disease.
Survival rates are calculated by tracking the percentage of patients who are alive at a certain point, typically five years, after their diagnosis. These rates provide an estimate of the likelihood of survival based on data from large groups of patients with similar characteristics and stages of cancer.
How can you interpret survival rates in the context of colorectal cancer with caution?
Individual prognoses may vary widely based on factors such as age, overall health, genetic factors, response to treatment, and access to healthcare.
Survival rates are general estimates and may not reflect the specific circumstances or outcomes for every patient
Advances in treatment options, such as surgery, chemotherapy, targeted therapy, and immunotherapy, continue to improve outcomes and may influence survival rates over time
Regular follow-up care and monitoring are essential for detecting and managing any recurrence or complications that may affect the prognosis
While survival rates offer valuable insights into the overall prognosis of colorectal cancer at different stages, they should be viewed as general estimates. Each patient’s journey with colorectal cancer is unique and personalised treatment plans and ongoing support from healthcare providers are crucial for optimising outcomes and quality of life.
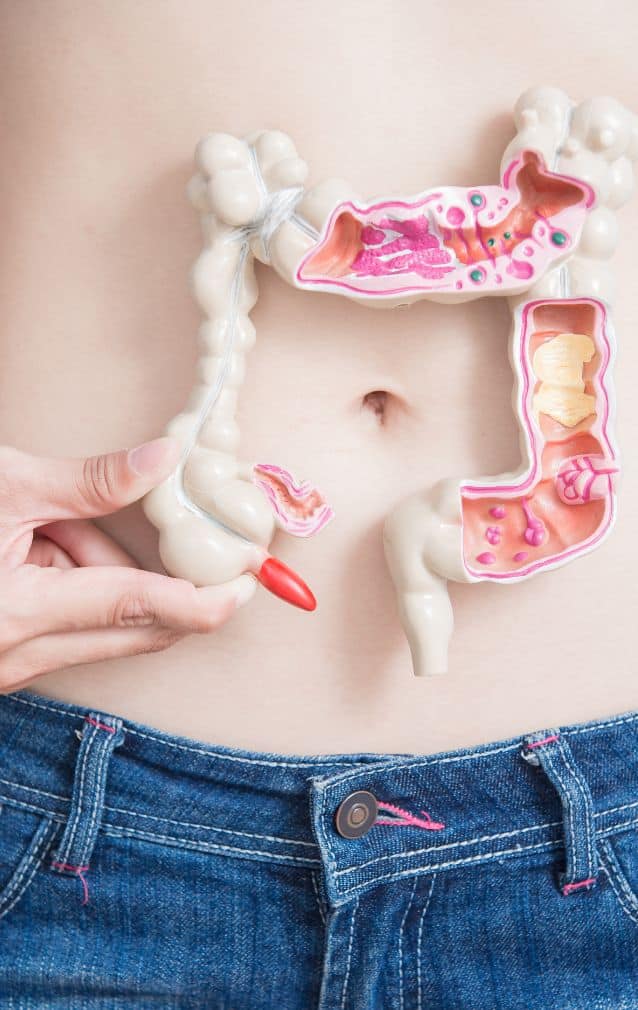
What are the positive factors that can impact cancer prognosis?
Regular screening tests, such as colonoscopies and FOBTs, can detect colorectal cancer at an early stage or even identify precancerous growths (polyps) before they become cancerous. Early detection allows for timely intervention, increasing the likelihood of successful treatment and better outcomes.
Over the years, there have been significant advancements in the treatment of colorectal cancer, including improvements in surgical techniques, chemotherapy regimens, targeted therapies, and immunotherapies. These treatment options offer more effective ways to manage the disease, reduce the risk of recurrence, and improve survival rates.
Adopting a healthy lifestyle can positively impact the prognosis for colorectal cancer. This includes maintaining a balanced diet rich in fruits, vegetables, whole grains, and lean proteins while limiting processed foods, red meat, and alcohol consumption. Regular physical activity and weight management also play a role in reducing the risk of colorectal cancer and improving overall health outcomes.
By prioritising regular screening, adopting healthy lifestyle choices, and maintaining open communication with healthcare providers, individuals can take proactive steps to improve their colorectal cancer prognosis and overall health outcomes. Early detection, timely treatment, and ongoing support are key to effectively managing the disease and achieving the best possible outcomes.
FAQs
Yes, the prognosis for colorectal cancer can vary widely among individuals due to factors such as age, overall health, genetic predisposition, tumour characteristics, treatment response, and access to healthcare. While survival rates offer general estimates, each patient’s prognosis is unique and may differ based on their specific circumstances.
Cancer staging, which categorises the extent of cancer based on factors like tumour size, lymph node involvement, and metastasis, is crucial in determining the prognosis for colorectal cancer. Staging helps healthcare providers assess the severity of the disease, plan appropriate treatment strategies, and estimate the likelihood of disease progression and survival outcomes.
Advancements in treatment options, including surgery, chemotherapy, targeted therapy, and immunotherapy, have significantly improved the prognosis for colorectal cancer over the years. These treatments offer more effective ways to manage the disease, reduce the risk of recurrence, and improve survival rates, particularly for advanced-stage cancers.
Speak to a specialist for a cancer prognosis
Seeking guidance from a specialist is crucial if you experience symptoms related to colorectal cancer. As one of the most prevalent cancers globally, it’s vital to address it promptly for the best chance of successful treatment. However, the approach to treatment depends on several factors, including the cancer’s origin, your overall health, lifestyle choices, and treatment preferences.
Dr. Suhirdan Vivekanandarajah is an esteemed specialist in gastroenterology and hepatology, practising in Sydney, Australia. With extensive expertise in colorectal cancer and its management, Dr. Vivekanandarajah offers compassionate care and tailored treatment plans for his patients.
Whether you’re experiencing symptoms, have concerns about your colorectal health, or require screening for early detection, booking a consultation with Dr. Suhirdan is a proactive step towards addressing the prognosis for colorectal cancer.
To take control of your colorectal health and explore personalised treatment options, schedule a consultation with Dr. Suhirdan Vivekanandarajah today.
