What is gastroscopy?
Gastroscopy, often referred to as an upper endoscopy, is a medical procedure conducted using a thin and flexible tube, also known as an endoscope, to examine the upper part of the digestive tract. The endoscope is inserted into the mouth, which travels down the oesophagus (food pipe) and into the stomach. The endoscope contains a light and camera that takes videos and images of your digestive tract.
Why are gastroscopies conducted?

A gastroscopy is conducted to analyse and examine the abnormalities, reactions, and symptoms of your digestive system and it can also be conducted to treat and diagnose types of cancer.
A gastroscopy can check the reason behind your digestive symptoms, such as:
Tendency to feel nauseous
Vomiting contents of blood
Chest pain and stomach aches
Constant sensations of heartburn
Passing dark stools along with blood
Inabilities and pain felt when swallowing
What can a gastroscopy treat?
A gastroscopy can sometimes also be used to treat problems within the digestive system. A gastroscopy can assist in:
Widening the oesophagus to help smooth digestion
Preventing internal bleeding from the stomach or oesophagus
Removing the growths of cancer cells within the digestive tract
Acting as a feeding tube which aids in swallowing and digesting
Identifying stomach or oesophagal cancer
A gastroscopy is performed to provide a diagnosis and evaluation of various gastrointestinal conditions. This can help identify and provide details on issues like ulcers, digestive inflammation, tumours, bleeding, causes of abdominal pain, inability to swallow, and unexplained weight loss.
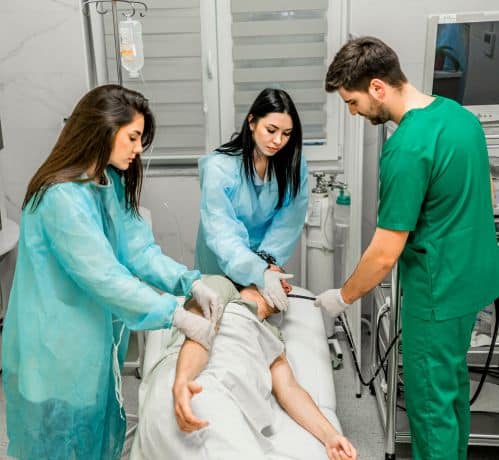
Gastroscopy preparation processes that a patient must follow
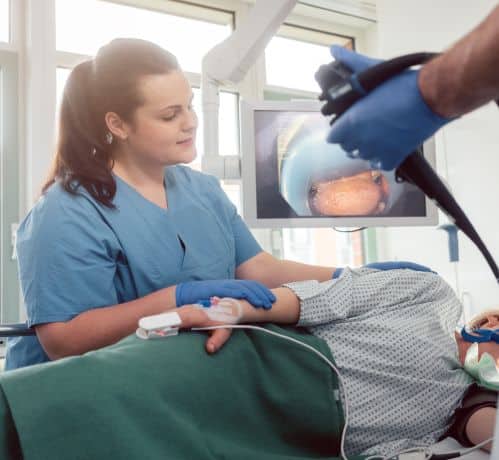
Before undergoing a gastroscopy, you will need to empty your stomach and digestive system, to ensure clarity in the endoscopy and to prevent you from vomiting during the procedure. It is important to stop consumption of food and fluid 6 hours before the endoscopy. Moreover, your specialist will advise you about procedure specifications.
Your gastroscopy clinic will send you a detailed briefing that will hold details on:
The wait period for the gastroscopy results
What foods and fluids to consume before your gastroscopy
Medicines you may be offered before having endoscopy preparation
How to prepare for the day of the gastroscopy
On the day of the gastroscopy, you will be able to have small sips of water; most often, your specialist will highlight how much water you can drink before the examination.
Your doctor will give you sedation and anaesthesia medications. Sedation is given to relax your nerves and body before a gastroscopy is conducted—this is likely to stay active in the body for about 24 hours.
It is safer to either remain in the hospital under the eye of your doctor or arrange for a caretaker, a family member, or a friend to keep watch over you. It is best to apply for leave the day after the endoscopy for symptoms of anaesthesia and the endoscopy to wear off.
Sedation or anaesthesia is administered to prevent you from having the urge to vomit during the process. However, this sensation should stop once the tube reaches your stomach. During the process, you are likely to experience bloating and feeling full.
The symptoms of sedation and anaesthesia include:
Nauseous feeling
Headaches
Slower heart rate
Low levels of pressure
Dizziness and confusion
Difficulty in passing urine and stools
The procedure of gastroscopy is likely to take around 15-45 minutes. However, the total time spent in the hospital under examination and during review and monitoring may take around 4 hours of your time. A gastroscopy should not be painful because you are under the influence of sedation and anaesthesia but if you do feel pain, you can ask the gastroscopy to be halted.
What is the process after a gastroscopy?
After the gastroscopy, your specialist or nurse may explain the results before you leave the hospital.
A follow-up appointment will be scheduled to talk about your gastroscopy results and discuss treatments.

FAQs
Typically, a colonoscopy is used for faecal transplantation. The solution containing donor faeces is poured into the colon as the colonoscope is withdrawn after being guided entirely through the colon by a gastroenterologist.
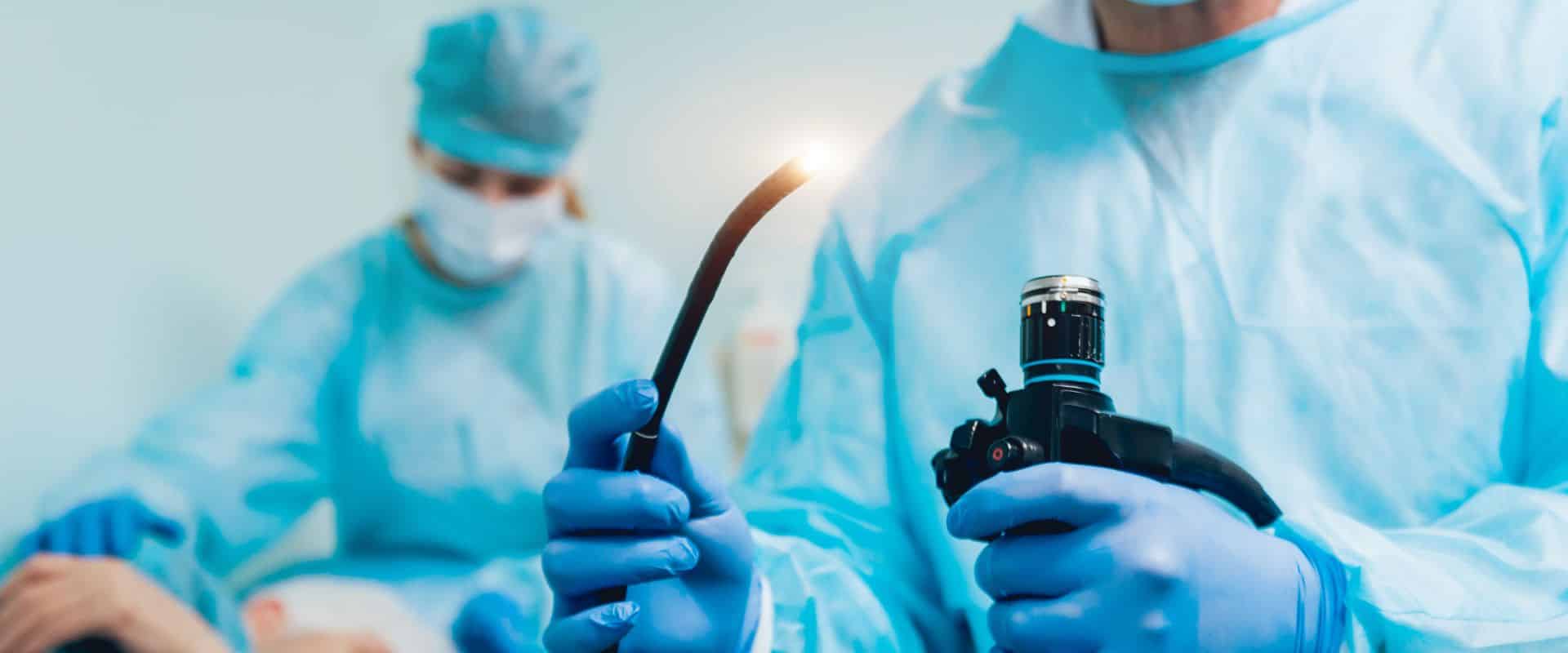
Before a gastroscopy, certain rules or guidelines must be followed; for example, fasting and medical adjustments made to the patient. However, it is important to have an in-depth consultation where your specialist is informed about your medical conditions and history before signing the consent form for a gastroscopy.
A typical gastroscopy does not require bowel preparation. Bowel preparation involves clearing out the intestines and is more commonly done with procedures like colonoscopies.
For a gastroscopy to be conducted, it is important to ensure that your stomach is adequately empty for the procedure. General guidelines that might be advised by your specialist are consuming clear liquids, avoiding solid foods, and staying away from alcohol and coloured beverages as these leave residue in the stomach or obstruct the clarity of the examination.
Speak to a specialist about getting a gastroscopy
Dr. Suhirdan Vivekanandarajah is a highly experienced and qualified gastrointestinal specialist based in Sydney, Australia. He has extensive experience in treating various areas of gastroenterology and has provided patients with phenomenal support and treatment for their medical needs for many years.
If you’re concerned about your gut health and want advice on gastroscopy preparation or an endoscopic evaluation, book a consultation with Dr Suhirdan today.
