What is IBS?
Irritable bowel syndrome (IBS) is a common disorder affecting the large intestine or colon. The disorder is chronic with symptoms of abdominal pain, discomfort, and an erratic change in bowel habits, among either diarrhoea, constipation, or alternation.
The exact cause is not clear, but it is believed to involve a mixture of factors, such as unusual contractions of the intestinal muscle, increased sensitivity to some stimuli, changes in gut microbiota, and changes in the communication between the brain and the gut.
Generally, it is a symptomatic diagnosis since there isn’t a clear-cut test for it; the symptoms manifest in varied levels from one person to the other and can also be spread far apart over a long period. While it does not incur permanent damage to the digestive system or increase susceptibility to other serious diseases, like cancer, IBS can seriously impair the quality of life of an individual and the daily functioning of that person.
Treatment may include simple lifestyle and dietary changes, stress management techniques, and medications that help control symptoms, such as antispasmodics, laxatives, or antidepressants. The physician may additionally advise a kind of therapy, such as cognitive-behavioural therapy (CBT) or gut-directed hypnotherapy, in the event of IBS patients needing help managing it.
What are the diseases treated with faecal transplantation?
For many gut and indigestion conditions, healthcare researchers have found that faecal transplantation is a possible treatment:
IBS is characterised by a range of symptoms that can vary in intensity and duration from person to person. The most common symptoms of IBS include:
Frequent diarrhoea and loose stools
Cramping and tenderness in the abdomen
Fast heart rate
Dehydration and quick loss of fluids
Fever and increased body temperature
Nausea and vomiting
Increased white blood cells
Kidney failure
Loss of appetite
Swollen and inflamed abdomen
Unexplained weight loss
Passing stools with blood
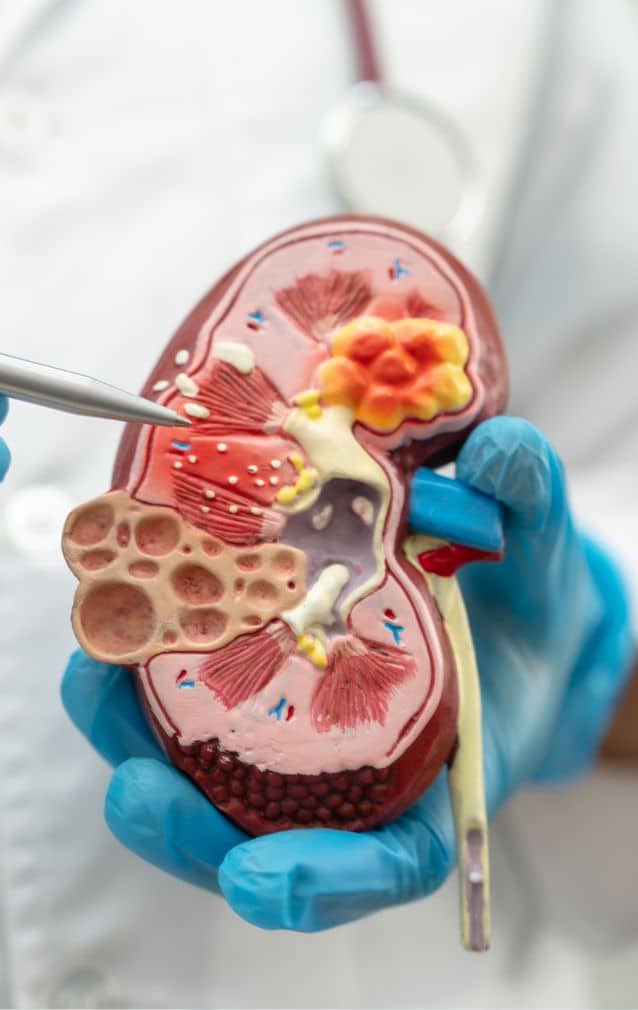
What is a stool transplant for IBS?
Stool transplantation, also known as faecal microbiota transplantation (FMT), is a procedure in which faeces containing a healthy balance of bacteria are transplanted from the gastrointestinal tract of a donor into a recipient. This method is primarily used to treat certain gastrointestinal diseases, such as recurrent clostridium difficile infection (CDI). Still, it has also shown promise in treating other diseases such as inflammatory bowel disease (IBD) and IBS
What are the aims of conducting a stool transplant for IBS?
The stool transplant for IBS aims to correct imbalances in the gut bacteria that may lead to symptoms of IBS. The aim is to increase gut health and reduce symptoms of IBS by transferring healthy bacteria from a donor.
The process is applied to instil healthy bacteria into the receiver’s gut so that, in turn, a more balanced microbiome may be restored. Otherwise, generally, a lack of balance in gut bacteria may contribute to IBS symptoms, and thus the transplant corrects the defect.
Better balance and diversity of gut bacteria to improve symptoms of IBS, like abdominal pain, bloating, diarrhoea, and constipation.
Stool transplants, in turn, would bring about enhanced overall gut health as a result of improved diversity and stability of the microbiome—aspects that can bring beneficial effects in digestion and the functioning of the gastrointestinal system in general.
Bearing this in mind, it should be emphasised that although these are the stool transplant goals in IBS, its efficacy and safety remain to be investigated phenomena, with more proof required to discern the long-term benefits.

What is the prevalence of IBS and its impact on daily life?
The symptoms of IBS can have a significant impact on daily life, affecting various aspects such as:
Work and productivity
Individuals with IBS may struggle to concentrate or perform effectively at work due to abdominal discomfort, frequent bathroom trips, or fatigue associated with their symptoms.
Social activities
IBS symptoms can interfere with social activities and outings, leading to anxiety or avoidance of certain situations due to fear and anxiety of experiencing symptoms in public.
Dietary restrictions
Many IBS patients are compelled to modify and change their diets to avoid triggering foods or substances that could worsen and aggravate their gastrointestinal symptoms.
Emotional well-being
Living with the unpredictable nature of IBS symptoms can take a toll on emotional and mental health, leading to stress, anxiety, depression, or feelings of isolation.
IBS is a common condition characterised by symptoms such as abdominal pain, bloating, diarrhoea, and constipation, which can significantly impact daily life and overall well-being. It’s important for individuals experiencing these symptoms to seek medical evaluation and support to effectively manage their condition and improve their quality of life.
The interference of IBS symptoms with social activities and outings goes beyond mere physical discomfort; it encompasses emotional challenges, relationship dynamics, and overall well-being. Individuals with IBS need to seek support, understanding, and effective management strategies to navigate these social challenges and lead fulfilling lives despite their condition.
How should you prepare for faecal transplantation?
Your specialist will need to be informed about your family history, drugs, allergies, and lifestyle before your transplant. Some specific preparation for a transplant will be advised by your doctor, who may advise that you stop having antibiotics for a while.
A clear liquid diet and an enema or laxative the day before the transplant may be advised by the doctor. Ensure that a responsible adult takes you home after the transplant is done and stays with you while you are healing.
What are the after-effects of a faecal transplant?
After undergoing a stool transplant, you’re likely to experience short-term side effects such as:
Bloating, intestinal gas, and belching
Leaking of the transplant solution through the anus and rectum
Cramping felt in the area of the colon whilst the transplant is ongoing
Constipation and tight stools because the specialist is likely to recommend anti-diarrhoea medication
However, these are of utmost seriousness; they depend on the patient, lifestyle, feeding, and age. The most serious side effects include:
Infections and viruses are most likely to be contracted from the donor of the stools; this is most likely to happen if there is no proper testing, scans, tests, and procedures carried out on the donor
Symptoms of pneumonia from the faecal transplant, or an infection, bleeding, and tears after conducting the colonoscopy or endoscopy from the transplant and the risks of undergoing anaesthesia
FAQs
While faecal microbiota transplantation (FMT), also known as a stool transplant, has shown promise in treating certain gastrointestinal conditions such as recurrent clostridium difficile infection (CDI), its effectiveness in treating IBS is still being studied. More research is needed to determine the factors that influence treatment outcomes and identify which patients are most likely to benefit from stool transplants. Some individuals may experience significant symptom improvement, while others may not respond as well.
The success rate of FMT for IBS is still a topic of ongoing research, and there is currently limited data available to determine a precise success rate. While some studies have reported positive outcomes with FMT for IBS, including improvements in symptoms. Success rates may be influenced by factors such as the specific characteristics of the patient’s IBS, the severity of symptoms, the composition of the donor stool, the method of FMT delivery, and other individual factors. IBS is a complex condition with diverse symptom patterns and underlying mechanisms, and what works for one person may not work for another.
It’s important for individuals with IBS who are interested in donating stool for FMT to discuss their eligibility with their healthcare provider. They can provide personalised guidance and recommendations based on individual circumstances and ensure that the donation process is safe and appropriate.
Speak to a gastro-specialist about getting a stool transplant for IBS
If you’re seeking expert guidance on faecal microbiota transplant (FMT) or colonoscopy, Dr. Suhirdan Vivekanandarajah stands as a premier gastrointestinal specialist based in Sydney Australia.
With extensive training and expertise in gastroenterology, Dr. Vivekanandarajah has a distinguished track record of providing top-tier care, addressing a wide spectrum of gastrointestinal concerns.
If you're experiencing concerns regarding your gut health or are contemplating the need for FMT or a colonoscopy, scheduling a consultation with Dr. Vivekanandarajah could offer invaluable insights and personalised treatment options tailored to your specific medical needs.
